Radiotherapy Treatment for Prostate Cancer
What is Radiotherapy for Prostate Cancer?
Radiation Therapy, also called Radiotherapy, is one of the main treatments for cancer.
Radiation Therapy is a safe and effective treatment for Prostate cancer and is designed to destroy or injure cancer cells so they cannot multiply.
Why is Radiation Therapy Used?
The aim of Radiation Therapy is to:
- Cure The Cancer – some prostate cancer can be cured by radiation therapy alone or combined with other treatments.
- Control of Prostate Cancer – radiation therapy can control some cancers by making them smaller or stopping them from spreading.
- Relieve Symptoms – if a cure is not possible, radiation therapy may be used to reduce cancer symptoms and prolong a good quality of life.
How Does Radiation Therapy Work?
Radiotherapy involves the controlled application of radiation to the cancer cells using high-energy x-rays, gamma rays, electron beams or protons to kill cancer cells using a machine called a ‘Linear Accelerator’.
Focusing the radiation on the area to be treated reduces the impact of treatment on healthy areas of the body. Cancerous cells are more susceptible to radiation than healthy, non-cancerous cells and while normal cells can also be damaged they usually recover.
Types of Radiation Therapy for Prostate Cancer?
There are two main types of Radiation Therapy:
- External Beam Radiation Therapy (EBRT) – involves a machine that aims radiation at your cancer. The machine moves around your body and sends radiation from many directions. Before you start treatment, your doctor will map out the exact location of your prostate. Then you will have treatment once a day, 5 days a week, usually for 4 to 8 weeks, often in combination with temporary androgen deprivation therapy (ADT). Each EBRT treatment session takes about 15 minutes.
There are different types of External Beam Radiation Therapy (EBRT).
- intensity- modulated radiation therapy (IMRT) – shapes the radiation beams to allow different doses to be given to different areas. Volumetric modulated arc therapy (VMAT) is a specialised form of IMRT that delivers radiation continuously as the treatment machine rotates around the body.
- Image-guided radiation therapy (IGRT) – uses a treatment machine that takes CT scans and x-rays at the start of each session to check that you are in the correct position for treatment. This improves accuracy and reduces the risk of side effects. Fiducial markers (usually grains of gold) may have been inserted into or near the cancer so they can be seen in the x-rays or scans and used to guide positioning.
- Stereotactic body radiation therapy (SBRT) – This is a newer treatment and is not widely available. SBRT is delivered in 5–7 treatments over two weeks. Not all prostate cancers are suitable for this very short-course treatment – you can discuss this with your radiation oncologist.
- Brachytherapy – is a type of internal radiation therapy in which a doctor places radioactive material inside the prostate. Brachytherapy is a choice for men with low-risk prostate cancer. There are two main types of brachytherapy used for prostate cancer,
- Low-dose Rate (also called LDR) and
- High-dose Rate (also called HDR)
Are You a Candidate for Radiation Therapy?
In general, radiotherapy is suitable if the cancer is still in the prostate gland and has not spread to other areas of the body.
A number of tests will be carried out to see if radiation therapy will help, including:
- Urinary and Bowel symptoms
- Previous Radiotherapy
- Checking pathology reports
- PSA Test
- Prostate MRI Scan
- CT scans of Abdomen and Pelvis
- Bone Scan
- PSMA-PET Scan
Radiotherapy Planning for Prostate Cancer?
Treatment is individually tailored to improve efficacy, relieve symptoms and to limit side effects.
The Radiation Therapy often involves three steps and is designed to help the radiation therapy team plan and work out the best way to deliver the treatment to your prostate while limiting radiation to the bowel and bladder.
Simulator Planning Session
- Measurements are taken by X-rays from the front and side while lying face down.
- Small marks are made for targeting
- It is important to try not to empty your bladder beforehand.
- This procedure requires no special preparation and is not painful.
Planning CT Scan
This takes place about a week after your Simulator Planning Session and is similar.
- The CT scan takes pictures of the prostate gland.
- It is important to try not to empty your bladder beforehand, but
Treatment Plan
The radiation therapy team will use the information collected during your Simulator Planning Session and Planning CT Scan to work out the best way to deliver your treatment.
Side Effects of Radiotherapy Treatment
The bowel and bladder lie next to the prostate gland and during Radiotherapy, some of the normal cells of the bowel or bladder may be damaged due to their proximity to the prostate.
Although care is taken so that radiation does not affect these areas, sometimes it is unavoidable.
Short-term side effects may include:
- A burning feeling when urinating or the need to urinate more often.
- Bowel movements may become looser and more frequent, and there may be spots of blood and discomfort when emptying the bowel.
- Many people may also feel a loss of energy and increased lethargy during radiation therapy but this should remedy soon after treatment.
- For most people side effects settle down within a month of completing treatment, although it may prolong for some.
Long-term side effects may include:
- A small number of men may develop long term complications from Radiation Therapy such as frequent rectal bleeding or other bowel problems.
- Some men may find that treatment affects their sexual function, including erectile dysfunction and discomfort or a lack of fluid during ejaculation.
- Side effects of radiation therapy differ between men and so it is impossible to determine who will have what side effects.
- If you suffer any side effects, it is important you let your doctor know as soon as possible so that appropriate help can be given.
SpaceOAR hydrogel
To reduce the risk of bowel or rectal damage Dr Kim can place SpaceOAR hydrogel. It’s a water-based soft gel implant that temporarily creates a small gap between the prostate and the rectum. This gap protects the rectum from radiation exposure during prostate radiation therapy, meaning fewer side-effects. SpaceOAR hydrogel stays in place for around three months. After that, it’s naturally absorbed by the body and passed out in your urine.
Resources are available to help manage any side effects experience.
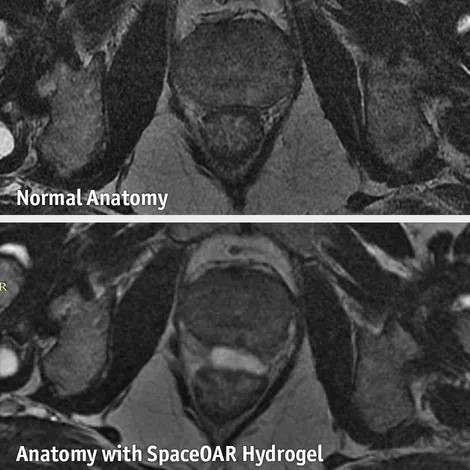
Before and After Placement of spaceOAR on MRI
Radiotherapy Treatment in Sydney
If you need Radiotherapy in Sydney, contact now!
